CMS released the proposed rules for 2021 this week. Below is a list of the changes that we believe will have the most impact on the urology practice. This list is not all-inclusive but more of an executive summary.
As we learn more we will continue to update you on the changes.
The Top 8 Changes Impacting Urology Practices
- The final rule will be released in December, not late October/ early November
CMS is going to invoke a protocol that allows them to post the final rule only 30 days before it goes into effect on January one, that’ll mean that the final rule is actually going to be posted early December. So we won’t have as much time to react. - Conversion factor decreasing by 10.6%
CMS is required to make changes to the physician fee schedule under a constraint of Budget neutrality. The change in codes and values related to E/M codes, noted later in this document, will result in an increased payment for E/M codes. Due to the volume of services reported under this code Medicare is projecting an increase in the overall cost to the system which is adjusted by lowering the conversion factor.
The good news is that urology as a specialty is projected to be up 8%. The projection is based on urologists as a group, as not all urologists bill for the same services individual, each urologist will be impacted differently.
- E&M Codes and Rules: the new code structure and significant documentation changes will go into as effect as planned
The decisions CMS made in 2020 and released in 2020 are unchanged and scheduled to be implemented in 2021. CPT codes for new and established patient visits in the office will undergo significant changes, as most are aware. As a reminder the changes include will only effect office visit codes and include:- Deletion of code 99201
- Change in documentation requirements will remove History and Physical examination bullet point requirements and require only medically appropriate HX and PE.
- MDM is changing and will drive the selection of most codes
- Time values and time definitions are changing
- Values will be increased for each level
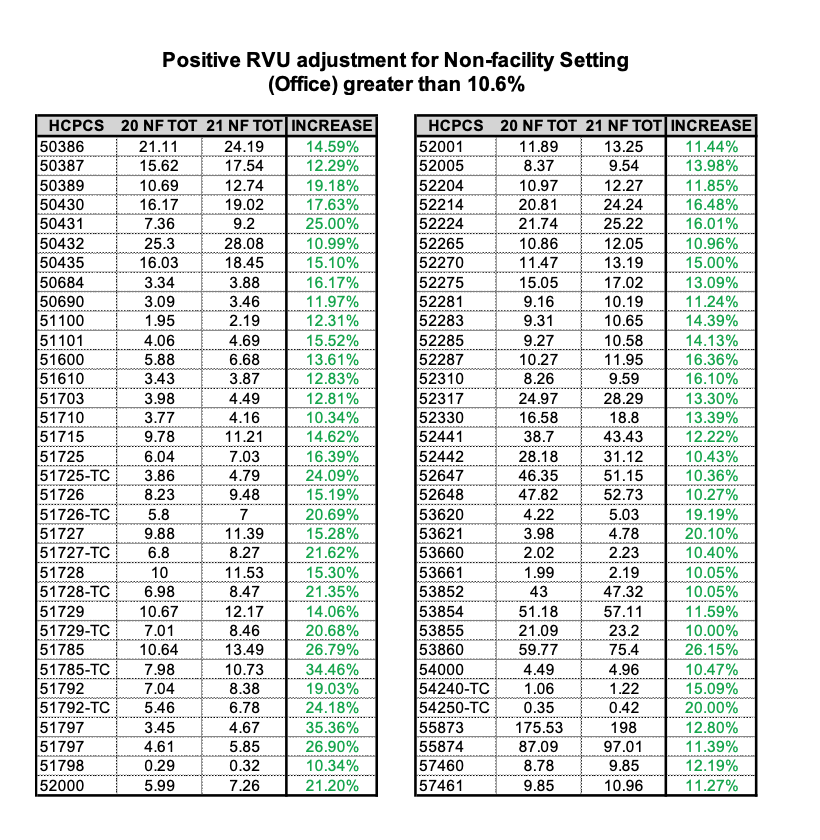
- RVUs for non-facility codes increasing enough to offset conversion factor decrease
Many high volume urology procedures RVUs are actually going up enough to offset or exceed that 10.6% conversion factor drop. So this includes services you provide in the office like urodynamics, Urolift, Rezume, many procedures done through the scope, including small bladder biopsies, and small bladder tumors.
- RVUs for facility procedures are not changing or changes will not offset the conversion factor decrease.
Practices with a significant amount of their income based on services provided in a facility will be negatively impacted. Income for practices that provide many or most of their services in the hospital or in the ambulatory surgical center will see a decrease in professional fees. RVU changes were minimal, so the initial impact on RVU based contracts will be minimal unless or until contract payments for amount per RVU are changed to mimic payments from Medicare.
- ASC payments are set to increase
There has been a bump in the ambulatory surgical center (ASC) payments generally. This increase may offset or impact practices owning or participating in ASCs as a net positive relative to professional fee decreases listed above.
- MIPs rule changes are minor but warrant further review.
CMS shifted more of the balance of MIPS onto the cost portion. It’s increasing from 15% to 20% and the overall minimum score is going to jump from 45 to 50. - Telehealth is going to continue with the same rules during the Public Health Emergency.
However, many of these changes will be carried forward when the PHE is over, however, Medicare by rule cannot cover Telehealth services when the patient is located in their home when the Public Health Emergency ends. Contact your congressman and encourage your patients to do the same, request that Medicare rules be changed to allow patients to receive telehealth from home. Telephone only codes 99441-99443 will not be covered after the PHE has ended. CMS has added a number of services to the list of covered Telehealth services and created a new category of services to explore further expansion of this list. Regulations are written in a way to indicate that the Public Health Emergency is expected to be extended into 2021.
CMS has added a lot of codes to the telehealth list and now there is going to be three categories of codes approved for telehealth
This is an executive summary of the items we identified that will have the most impact on the urology practice. As we continue to unpack the 1400 pages we will release another PRS Alert if we identify additional impactful proposed rules
Download the PDF: Positive and Negative 2021 RVU adjustment for Non-facility and Facility Urology Codes 50000 – 58000